Subscribe to our blog for all the latest news, updates, and events from MMA and our partners
Subscribe
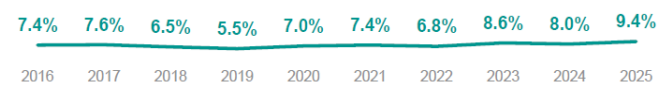
Employers face meaningful health cost increases in 2026 (estimated ~6.5%–10%+), which pushes up premiums, out-of-pocket costs, and budget uncertainty for individuals and companies.
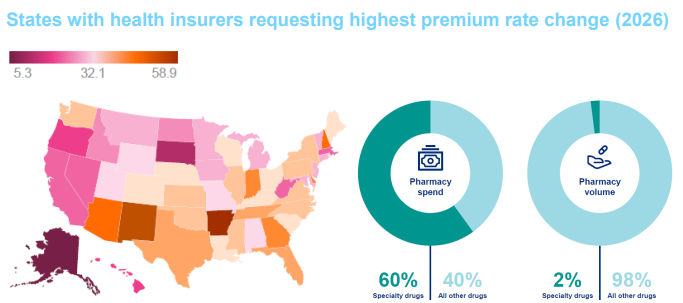
Much of the increase is coming from specialty medicines (especially oncology drugs) and the rapid rise of GLP-1 drugs used for weight loss and diabetes. These drugs are expensive, often ongoing, and are shifting pharmacy spending dynamics (Marsh & McLennan Agency; RAND analysis on GLP-1 use)
(https://www.rand.org/pubs/research_reports/RRA4153-1.html).
Pharmacy cost trends were 2.5 points higher than medical cost trends in 2025. The specialty pharma market grew from $92.5 billion in 2023 to $129.23 billion in 2024. It is expected to reach $965.5 billion by 2030.
Health spending is up across medical and pharmacy lines; specialty drugs account for a large share of pharmacy dollars even though they’re a small share of prescriptions.
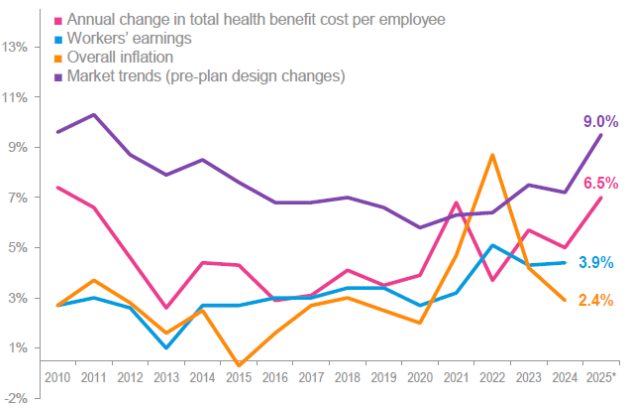
Action: Ask your broker/benefits team about targeted cost levers (specialty drug strategies, site-of-care steering, stop-loss design).
GLP-1s and other specialty therapies are major cost drivers; usage has surged. Employers are tightening access and adding prior authorization, lifestyle requirements, or outcomes-based contracting to manage use and cost.
GLP-1 medications are rapidly changing how conditions are managed. Originally prescribed for diabetes, they are now used to treat a wide variety of conditions, both off-label and with FDA approval.
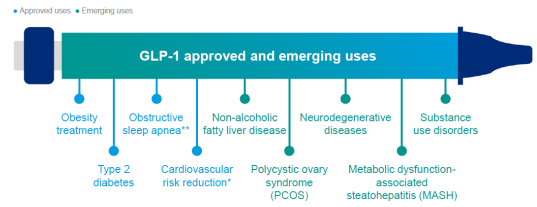
11.8% of U.S. adults used a GLP-1 medication in 2025 to lose weight or treat chronic conditions like diabetes or heart disease, while 14% reported interest in starting treatment.
Action: Review PBM contracts, require transparent pass-through pricing, consider biosimilar-first
approaches and step therapy where clinically appropriate.
New federal transparency emphasis offers more pricing data for plan sponsors to negotiate smarter networks and steer members to lower-cost, high-quality providers (White House price-transparency
order: https://www.whitehouse.gov/presidential-actions/2025/02/making-america-healthy-again-by-empoweringpatients-with-clear-accurate-and-actionable-healthcare-pricing-information/).
Action: Ask your broker for network benchmarking and clarity on how transparency data was
adjusted/validated before you make plan changes.
Review pharmacy contracts now (PBM transparency, biosimilar strategy, prior authorization rules).
Re-run renewals with scenario modeling that includes GLP-1 uptake and specialty oncology cases.
Audit plan communications to reflect OBBBA changes (HSA/DPC/FSA/Trump Accounts) and upcoming state mandates (e.g., fertility/IVF mandates). (OBBBA text: https://www.congress.gov/bill/119th-congress/housebill/1/text/pl).
Expand navigation, mental fitness coaching, and eldercare supports — high perceived value, often lower cost.
Insist on AI governance and training before rolling out employee-facing tools
EHB 2026 Trends Presentation — Marsh & McLennan Agency LLC
2026 Employee Benefits Market Outlook — Zywave / Marsh McLennan Agency
5 Employee Benefits Trends Shaping 2026.pdf — Zywave
2026 EHB Trends Placemat.PDF — Marsh & McLennan Agency LLC
Subscribe to our blog for all the latest news, updates, and events from MMA and our partners
SubscribeCopyright © 2026 Marsh & McLennan Agency LLC., All Rights Reserved.